Edit Content
Care that sees the woman, not just the risk
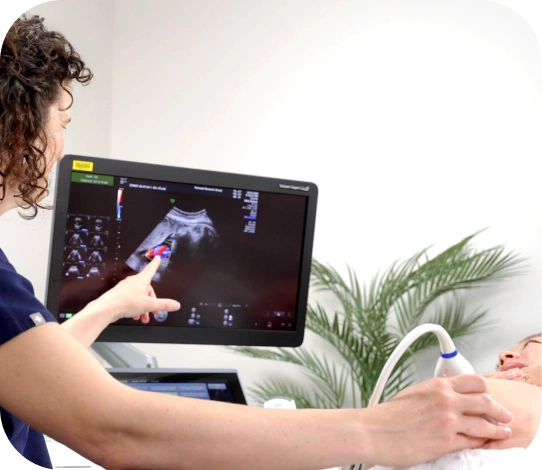
Learning that your pregnancy is considered high-risk can feel confronting and overwhelming. You may have entered pregnancy with a known medical condition, or complications may have arisen unexpectedly. Either way, it’s normal to feel unsettled when the path forward suddenly feels more complex.
As an obstetrician in Melbourne with a special interest in high-risk pregnancy care, I understand that behind every diagnosis is a woman who wants what every expectant mother wants: a safe pregnancy and the best possible start for her baby. The difference is simply that your journey requires closer monitoring, thoughtful planning, and personalised support.


When you’re ready, I would be honoured to support you through your pregnancy from my private consulting suite at The Royal Women’s Hospital in Parkville. Together, we’ll take the time to understand your circumstances and create a care plan that feels informed, considered, and right for you.
If you’d like to book a consultation, I look forward to meeting you and walking this journey alongside you.
A high-risk pregnancy is one where you or your baby require closer monitoring and specialist care to support the best possible outcomes. This may be due to a medical condition that existed before pregnancy, or a complication that arises along the way.
Importantly, the term high-risk does not define you or your pregnancy. It simply signals the need for more attentive, individualised care.
Women from Melbourne and beyond choose to consult with me when they are navigating:


If you have a pre-existing medical condition, pregnancy can add an extra layer of complexity. Medications may need adjusting, symptoms can change, and your condition may influence your baby’s growth and wellbeing.
Because no two high-risk pregnancies are the same, your care will never be one-size-fits-all. Your monitoring and management will be thoughtfully tailored to your individual health needs and circumstances. If concerns arise or complications develop, we can respond early and appropriately.
Throughout your pregnancy, I will take the time to explain your options clearly, guide you through the risks and benefits, and ensure you understand what’s happening and why. You will be actively involved in every decision — your questions are welcomed, and your voice truly matters.
Ideally, if you’re planning a pregnancy and have a known medical condition, we begin working together before conception through pre-pregnancy counselling. This allows time to carefully prepare and gives you the best possible foundation for pregnancy. Together, we can:

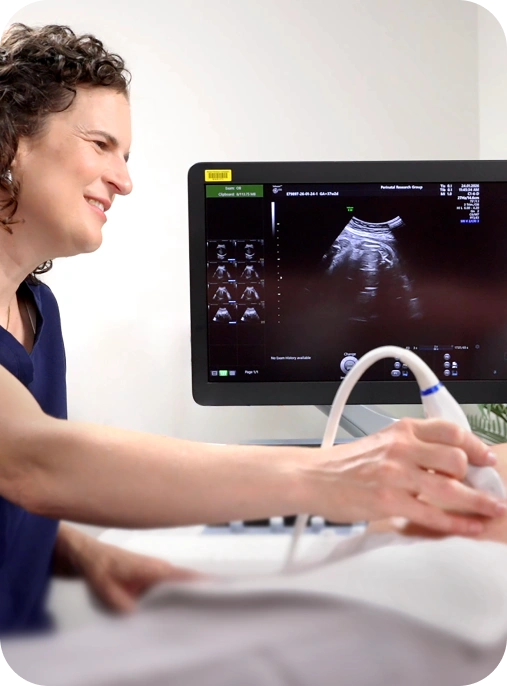


We begin with a comprehensive review of your medical history, current health, and any pregnancy-related risk factors. From there, your care is tailored to your individual needs and may include a higher level of monitoring and coordination.
Pregnancy with a pre-existing medical condition often involves more frequent appointments, additional testing, and closer collaboration with your broader healthcare team. This isn’t about being overly cautious — it’s about anticipating potential issues early and supporting the safest possible outcomes for you and your baby. Depending on your circumstances, your care may include:
Throughout this process, the focus remains on personalised, proactive care — with clear communication, continuity, and your wellbeing at the centre of every decision.
Managing a pregnancy alongside a pre-existing medical condition is never something you should navigate alone. I work closely with your GP, treating specialists, and wider healthcare team to ensure your care is coordinated and everyone is aligned.
You shouldn’t have to act as the go-between for multiple doctors or worry about whether information has been shared. I take responsibility for communication and coordination, so your care feels seamless, considered, and well supported — allowing you to focus on your pregnancy with confidence.
Every medical condition affects pregnancy differently. Below are some of the conditions I most commonly support women through, with care tailored to their individual needs:
Diabetes in pregnancy requires careful blood sugar monitoring, medication or insulin adjustments, and regular ultrasound scans to monitor your baby’s growth. Appointments are often more frequent, and in some cases, birth may be planned a little earlier to optimise outcomes.
Pregnancy naturally places extra demands on the cardiovascular system. Blood pressure requires close monitoring, some medications may need adjusting, and we remain vigilant for conditions such as pre-eclampsia to ensure early detection, prevention and management.
Autoimmune conditions can behave unpredictably during pregnancy and in the postpartum period. Some improve, while others may flare. Monitoring disease activity, adjusting medications safely, and assessing any impact on your baby are key components of care.
Pregnancy increases the workload on the kidneys. Regular kidney function tests, blood pressure monitoring, and close collaboration with your nephrologist help ensure both your health and your baby’s wellbeing are carefully supported.
If you have a history of blood clots or a diagnosed clotting disorder, blood-thinning medication may be recommended during pregnancy and after birth to reduce risk and support a safe outcome.
Seizure control remains essential during pregnancy, while also minimising any potential risks to your baby. I work closely with your neurologist to review medications and maintain the safest possible balance throughout pregnancy.
Your mental health is just as important as your physical health. If you are taking antidepressants, mood stabilisers, or anti-anxiety medications, we’ll carefully discuss whether continuing, adjusting, or changing treatment is appropriate — always prioritising both your wellbeing and your baby’s safety.



Birth can look different when a pregnancy is considered high-risk. You may need to deliver earlier than originally expected, and in some situations, a planned caesarean section may be the safest option for you and your baby. In some cases, your baby may benefit from access to neonatal intensive care after birth. While my consultations take place in my private rooms at The Royal Women’s Hospital in Parkville, I provide birth care at Frances Perry House, allowing for continuity and familiarity throughout your pregnancy journey.
As an obstetrician in Melbourne, I work closely with you to develop birth preferences that honour your wishes while thoughtfully considering medical needs and safety. At times, this involves open and honest conversations about why certain options may not be recommended. I am committed to explaining the reasoning clearly, answering your questions fully, and ensuring you feel listened to and supported in every decision.
If you have a pre-existing medical condition, pregnancy can add an extra layer of complexity. Medications may need adjusting, symptoms can change, and your condition may influence your baby’s growth and wellbeing.
As a Melbourne obstetrician with a special interest in complex and high-risk pregnancies, I provide the closer monitoring your care may require — while never losing sight of what matters most. You are still a woman growing a baby, experiencing the physical and emotional changes of pregnancy, and you deserve care that recognises the whole picture.
High-risk does not mean something is wrong — it simply means your pregnancy needs more thoughtful attention, careful planning, and personalised support. I am committed to providing this in a calm, caring, and unhurried environment. If you’d like to enquire about care, please complete my contact form and I will be in touch.

© Dr Carin Black. All Rights Reserved.